When attempting to achieve interdisciplinary expert consensus, experts are actually a problem. They are more than just individuals who know a lot in their respective fields. They represent the scientific stance of their discipline or academic community. In interdisciplinary discussions, experts bring more to the table than their personal opinion and wisdom. They bring their role and responsibility within their peer group into the discussion – connected with a certain weariness whether their peers would be happy about a consensus that usually contains some sort of pragmatic compromise.
This challenge is encountered aside from the actual question – be it in ethics commissions, technology impact assessments or medical guidelines – experts usually do not have much room to maneuver to find common ground for interdisciplinary compromise or consensus. Experts also are reluctant to follow majorities. Experts from scientific communities prefer a preciseness that despises watered-down middle grounds. And very often, the language each discipline uses and the differing emphasis on certain aspects of the problem further exacerbate misunderstandings and conflicts. Not to speak of competition between disciplines – be it for patients and preferred treatments or for funding and public recognition.
Still, interdisciplinary expert consensus is what you want to achieve: to clarify possible future developments, to steer and legitimize policy decision making, to move medical communities to change therapeutic standards or consider clinical questions in a broader perspective. And you want exactly those community-flagships, knowing that their maneuverability is limited.
A threefold approach can help:
Lever 1: Understand the rationales behind a certain stance or emphasis. Use a qualitative approach, questions and inquiries. Understand the professional beliefs and cater to them. Make the different positions understood by each participant. Sometimes coining new terms helps, widening the scope and bringing more aspects into the game. Or going into detail to find pragmatic solutions when a clash of belief systems proves not to be fruitful. Let the experts explain constraints they encounter in their daily work. This way you create shared understanding.
Lever 2: Build a sense of a common goal that a consensus may contribute to. Improving patient care to a certain degree even if not 100% from an ideal perspective of one discipline makes it worthwhile to stay on board. Sustainable urban planning, albeit not yet perfect from an ecological standpoint, will be broadly supported as long as it constitutes an overall progress. In conflicts try to avoid black-and-white decision making and steer towards gradual verdicts.
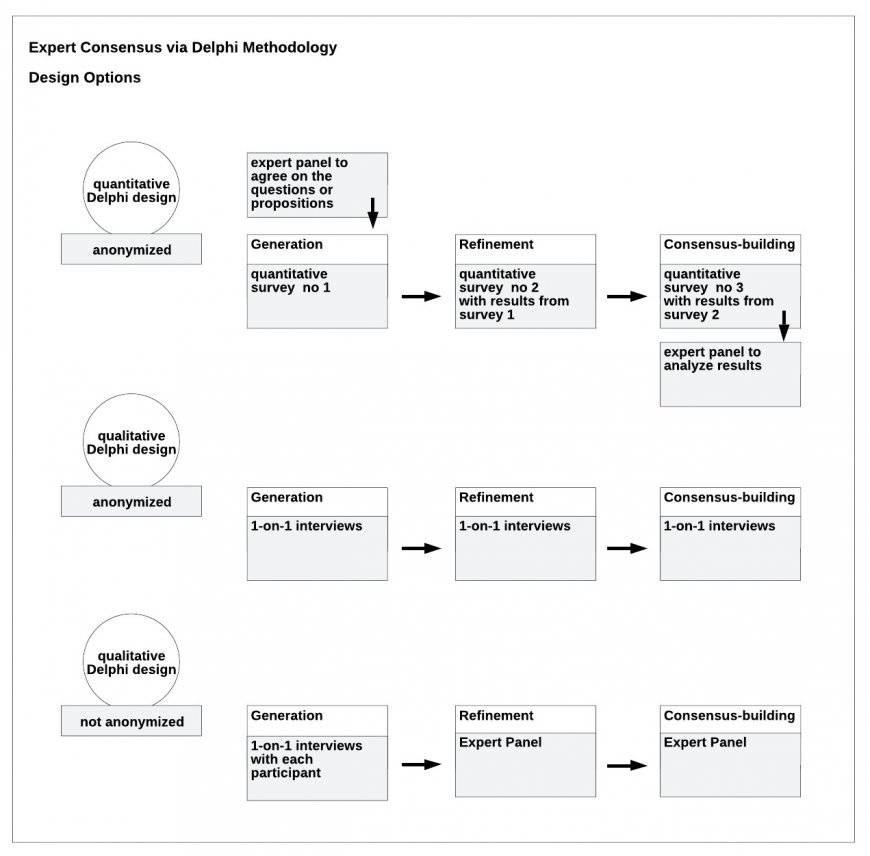
Lever 3: Design a stepwise process in consecutive rounds that build on one another. Decide on quantitative and qualitative elements. Qualitative elements facilitate expert consensus. Employ a first round of individual interviews: this can mitigate the risk of early-on confrontation. Create procedural satisfaction – it prepares the ground to accept an outcome even if participants need to make relevant concessions.
The Delphi methodology is designed for exactly that: giving a procedural design to develop interdisciplinary expert consensus even on very controversial questions. On-point design, professional moderation and simultaneous visualization of the expert discussion are the relevant success factors. Experts may still be a challenge for expert consensus – but with the right process you can definitely rise to this challenge!